- What is In-Vitro Fertilisation (IVF)?
- What is IVF with Life Whisperer Viability?
- What is Intra-Cytoplasmic Sperm Injection (ICSI)?
- Who is Suitable for IVF?
- IVF / ICSI Procedure
- Freezing of Extra Embryos
- Fertility Clinic Success Rates
- What Are The Risks Of IVF Treatment?
- Neonatal Insurance for Assisted Reproductive Programme (ARP) Treatment
What is In-Vitro Fertilisation (IVF)?
IVF is a process by which egg cells are fertilised by sperm outside the body. During IVF treatment, the eggs and sperms are put together in a petri dish. By natural selection, the egg will usually allow only one sperm to enter. This usually results in fertilisation of the egg. After in-vitro fertilisation, the embryos are allowed to grow for a short period of time before being placed into the uterus. A successful pregnancy can be confirmed about two weeks later.
IVF with Life Whisperer Viability
With Life Whisperer Viability, a non-invasive artificial intelligence (AI) system, embryologists can analyse the quality of embryos with more precision and decide which ones to transfer or freeze.
Watch: How Life Whisperer Viability Works

Frequently Asked Questions (FAQs)
Life Whisperer Viability has been trained to assess over 20,000 globally-sourced two-dimensional embryo images.
Some embryos have complex features that are difficult to detect and invisible to the human eye. Life Whisperer Viability harnesses AI to identify morphological features that affect the quality of embryos, and help embryologists select those that are more likely to result in pregnancy.
Patients can look forward to a shortened time to pregnancy with this evidence-based IVF treatment.
Couples who are eligible for IVF treatments can opt to add on the Life Whisperer Viability service. Find out if you qualify for IVF here.
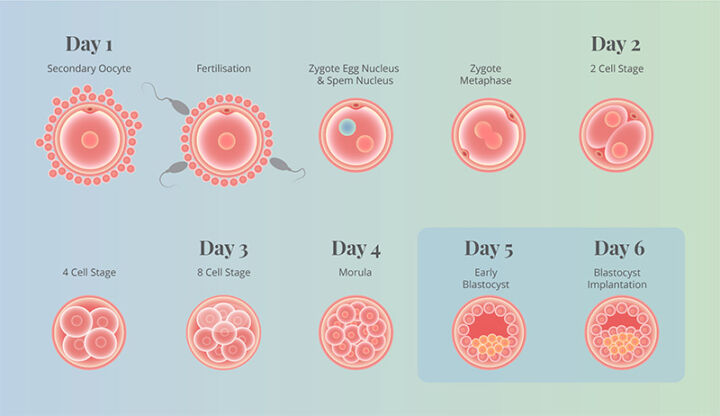
After the oocytes are fertilised in the IVF laboratory, they are cultured and kept in incubators to help them grow and develop into blastocysts (advanced embryos) before they are transferred to the uterus or frozen for future use.
On day five, embryologists will take photographs of your embryos (blastocysts only). The images will then be uploaded onto Life Whisperer Viability (web-based application).
Based on a value from zero to 10, where 10 denotes the highest quality with the highest potential, embryos are analysed in real-time with results generated in less than a minute. The results will be used to help embryologists make embryo selection.
No. Although Life Whisperer Viability leverages AI to assess embryos, it is a clinical decision support tool that removes subjectivity and provides objective assessments of embryos. This helps our embryologist make the best clinical decisions and decide which embryo to transfer for the best outcome.
Life Whisperer Viability is compliant with HIPAA, GDPR, and ISO 13485. Information is saved in the local cloud server so data remains safe in the region of origin. Data is encrypted to the highest standards.
Keen to find out more about how Life Whisperer Genetics can help you begin your fertility journey? Call 6311 1250 or make an appointment to consult our specialists at Raffles Fertility Centre.
What is Intra-Cytoplasmic Sperm Injection (ICSI)?
In cases where the husband has very poor quality sperms, or if you have had difficulties with fertilisation in the past, ICSI may be recommended. Older women will often need this as fertilisation is poorer with older eggs. ICSI involves injecting a single sperm into each egg to allow fertilisation to occur in the laboratory. The average fertilisation rate with ICSI per mature egg is 70 per cent in our laboratory at Raffles Fertility Centre.
Who is Suitable for IVF?
Married couples with any of the following conditions are suitable for IVF treatment:
- Irreparably damaged or blocked fallopian tubes
- Cannot conceive with simpler methods of treatment for conditions such as ovulatory dysfunction, immunological problems or unexplained infertility
- Severe endometriosis
- Sperm disorders
IVF / ICSI Procedure
IVF programmes utilise Controlled Ovarian Stimulation, which results in more eggs, and hence a better chance of pregnancy.
Step 1: Drug Treatment to Stimulate Multiple Eggs to Mature
Short Protocol: GnRH Antagonist Protocol
The GnRH Antagonist protocol is the standard protocol used at Raffles Fertility Centre.
The antagonist protocol usually begins with the onset of your menses, either on Day 2 or 3. GnRH (e.g. Gonal F, Puregon or Menopur) are injected daily into the subcutaneous tissue of your thigh or abdomen to stimulate the growth of the follicles in the ovaries.
During this phase, you and your husband need not abstain from sexual intercourse after 4 to 6 days. Daily GnRH Antagonist injection is added. The combinations of both these types of injections are given daily in order to allow multiple eggs to develop whilst preventing ovulation. Depending on your ovarian response, other medications may also be given to optimise the ovarian response.
Step 2: Monitoring of Ovarian Stimulation
After several days of gonadotrophin injection, an ultrasound scan is performed to determine the number and size of the growing follicles. This is repeated till the follicles reach the desired size. Generally this phase takes 8 to 12 days of injections. Blood tests may be needed to measure the hormone levels and your medications adjusted according to your response.
When the follicles have reached the desired size, an injection is given to trigger ovulation and the final maturation of the eggs. The egg collection is scheduled about 35 to 37 hours after this trigger injection.
Step 3: Egg Collection
The egg collection is performed in our fertility operating room, and takes between 15 and 30 minutes. The eggs are collected through a special needle attached to an ultrasound vaginal probe. Overnight fasting is required before you come for the procedure. A mild sedative will be given to you as only minimal discomfort will be experienced during the procedure. After the egg collection is completed, you will be observed for a few hours before you can return home.
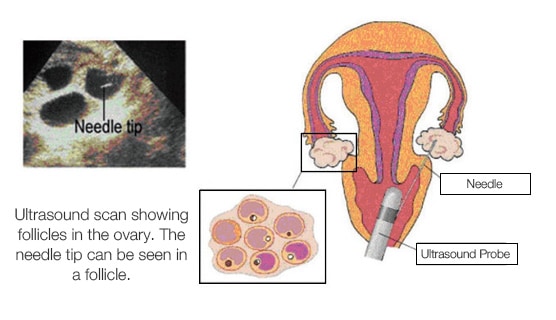
It is important to understand that not all follicles will necessarily contain an egg and that some eggs may not be ripe enough for fertilisation.
Step 4: Sperm Preparation
On the day of the egg collection, your husband needs to produce a fresh masturbated semen sample.
Step 5: Fertilisation
Routine IVF
The sperms are added to the collected eggs in a dish to allow fertilisation to occur by natural selection in the laboratory. A check to confirm that fertilisation has occurred is carried out the following day, and the embryologist will inform you of the result. In about 10 per cent of couples, fertilisation may not have occurred at all.
Intra-Cytoplasmic Sperm Injection
ICSI will be performed on the day of egg collection. During ICSI, a single sperm will be injected into each egg via a micro-needle. On the following day, a check is made to confirm that fertilisation has occurred. The embryologist will inform you of the result.
At Raffles Fertility Centre, most of the first cycles will have a combination of IVF and ICSI performed if enough eggs are collected and the sperms are of sufficient quality. This will help to determine whether there is a fertilisation problem.
Step 6: Embryo Transfer
If fertilisation is successful, the embryos will be placed into your uterus. Before the embryo transfer, you will be encouraged to drink two to three glasses of water to help facilitate the procedure.
The embryo transfer is done with a fine catheter and you will be asked to consume medication to enhance the chances of the embryos implanting.
Your IVF Specialist will discuss with you the number of embryos to be replaced into your uterus and the timing of this procedure.
You will be able to see your own embryos in the dish in which the embryos were grown before the embryos are placed into your uterus. This procedure is done with a fine catheter and is usually painless.
You may go home shortly after the embryo transfer, and will be given daily medications to support the lining of the uterus and to enhance the chance of the embryos implanting.
There is no restriction on food intake, work or sexual intercourse during this period. Resting in bed more than usual has not shown to increase the success rate of embryo transfer.
Freezing of Extra Embryos
A proportion of patients may have excess good quality embryos. These may be frozen for future use. Patients do not need to undergo Controlled Ovarian Stimulation and egg collection again for cycles using thawed frozen embryos.
Fertility Clinic Success Rates
Our overall clinical pregnancy rate is about 43 to 51 per cent per cycle. Additional frozen embryos further enhance the pregnancy chances in many of our patients.
Generally, patients who are below 35 years old have a better pregnancy chance. However, your chances of success will depend very much on your own individual circumstances.
Make an appointment online or contact the fertility clinic to consult a fertility specialist.
What Are The Risks Of IVF Treatment?
- Cancellation of the treatment may occur due to poor response of follicles to medications.
- Less than 1 per cent of patients might experience Ovarian Hyper Stimulation
- Syndrome. This warrants medical attention but can be treated.
- Miscarriage happens in about 20 per cent while an ectopic pregnancy (a pregnancy occurring outside the uterus) rate is about 5 per cent.
- When more than one embryo is placed, there is a 10 per cent chance of twins while chances of triplets are under 1 per cent. If this happens, there is an increased risk of miscarriages, pre-term birth & smaller babies.
- Egg collection has little risks and complications like bleeding from the ovaries, uterus or adjacent blood vessels and injury to the intestines rarely occur. In such occasions, further treatment may be necessary.
Make An Appointment
Make an appointment online or contact the fertility clinic to consult a fertility specialist. Under Specialist Appointment Details, select "Assisted Reproductive Medicine" or "Obstetrics, Gynaecology & Fertility".
Make an enquiry. We will get back to you within 2 working days. You can reach us at 6311 1250.