What is Temporomandibular Joint Disorder?
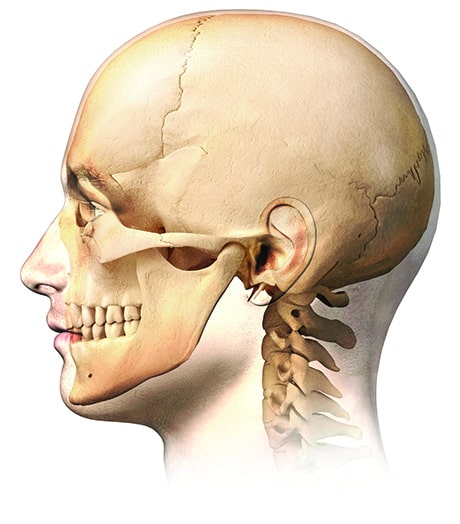
What is the Temporomandibular Joint?
The Temporomandibular joint (TMJ) connects your lower jaw (mandible) to your skull and is situated on either side of your head in front of the ears. It is one of the most frequently used joints in your body and probably the most complex. Being a modified hinge joint, it can move side to side as well as up and down allowing you to chew, talk and yawn. Its movement and position are controlled by muscles and ligaments attached to and surrounding it.
Signs and Symptoms of TMD
- Headaches
- Ear pain, blocked feeling, ringing sounds, partial hearing loss and dizziness
- Jaw pain – painful TMJ or chewing muscles located in temples and cheeks
- Jaw joint sounds – clicking, popping and grating sounds
- Jaw function difficulty – problems chewing, yawning and talking
- Abnormal jaw opening – limitation, asymmetrical movement, catching and locking
- Bite problems
- Neck and shoulder pain
TMD related pain, dysfunction and disability can significantly affect your quality of life.
What causes TMD?
Although there are specific reasons (eg trauma, degenerative arthritis) for some TMD, as a group they have no common cause and are usually the result of multiple contributing factors.
These include:
- Bruxism
Unconscious grinding and clenching of the jaws during sleep or when awake - Trauma/injury
Blows to face and/or jaws, biting on extremely hard food or an unexpected hard particle, extremely wide jaw opening - Habits
Regular gum chewing and eating only on one side
- Poor bite and jaw relationships
Poorly aligned teeth and skeletal problems - Medical conditions
Systemic arthritis and certain neurological conditions - Stress and anxiety
- Psychological conditions
Depression and somatisation
How is TMD treated?
Treatment largely depends on the kind of TMD that you are suffering from. Comprehensive history taking, physical examination and mental wellness screening (where applicable) is essential for complete diagnosis.
Routine or special TMJ X-ray techniques like MRI and CT scans are sometimes needed for diagnosing TMJ condition.
Treatment goals are to decrease pain, decrease adverse loading to jaw joints and muscles, restore function, restore normal daily activities and improve your quality of life.
Treatment usually starts with conservative therapies which do not invade the tissues of the face, jaw or joints and includes:
- Education and self-care
- Behaviour modification of harmful habits
- Psychotherapy including stress management and relaxation techniques
- Medications
- Physical therapy (e.g. TENS, ultrasound)
- Dental splint therapy
If your disorder does not improve with conservative methods, escalating to the next level of management is needed depending on the cause of your TMD. This includes, TMJ lavage, bite (occlusal) therapy or open joint surgery.