Tuberculosis
Tuberculosis, or TB for short, is a disease caused by a bacteria called Mycobacterium tuberculosis. TB can occur in any part of the body, but it most commonly affects the lungs (pulmonary TB). TB, which affects other organs outside the lungs, such as lymph nodes, bone or brain (extrapulmonary TB) is less common.
How Prevalent is TB?
Number of cases and distribution of tuberculosis infection by site, Singapore residents1 2011 – 2020
| Year | Lung | Other Sites | Total |
| 2011 | 1309 | 224 | 1533 |
| 2012 | 1359 | 201 | 1560 |
| 2013 | 1249 | 171 | 1420 |
| 2014 | 1220 | 234 | 1454 |
| 2015 | 1271 | 227 | 1498 |
| 2016 | 1353 | 264 | 1617 |
| 2017 | 1302 | 234 | 1536 |
| 2018 | 1309 | 238 | 1547 |
| 2019 | 1184 | 214 | 1398 |
| 2020 | 1124 | 246 | 1370 |
Source: Ministry of Health
1Residents refer to Singapore Citizens and Permanent Residents.
Recent events on TB situation in Singapore
MOH was notified on 2 March 2022 of seven TB cases involving residents of Block 2 Jalan Bukit Merah, who were diagnosed between February 2021 and March 2022. All seven individuals live in different units of Block 2 Jalan Bukit Merah. The cases were immediately started on treatment following diagnosis.
Genetic analysis and links, established in April 2022, revealed that all seven cases have similar genetic make-up. This suggests that these cases were linked by spread from one or more common sources. Investigations into the cases did not reveal any common links, other than that they live in the same block. The cases did not know or interact with one another, or congregate at the same common areas, and had also not identified each other as close contacts.
Therefore, as a precaution, MOH had offered TB screening to current and former residents, as well as stallholders, shop owners and their employees at that location.
Although TB rates have dropped since the introduction of highly effective medication in the 1960s, the disease continued to be a global public health problem. In 2021, there were 1,306 new cases of active TB cases among Singapore residents. This is lower than the 1,360 cases in 2020. The incidence rate was 32.8 cases per 100,000 population in 2021, compared to 33.6 cases per 100,000 in 2020. Older age groups (above 50 years old) and males continue to make up a significant proportion of the new active cases.
How Does TB Spread?
TB bacteria is passed through the air when someone who is affected with the active pulmonary (lung) TB disease coughs or sneezes. Those around the infected person for prolonged periods of time and those who breathe in the bacteria may be infected. As it is an airborne infection, people cannot get infected with TB through handshakes, sitting on toilet seats, sharing dishes or utensils.
Will Those Who Get Exposed to the Bacteria Develop the Same Symptoms?
Most healthy people exposed to the TB bacteria do not get infected, and active TB disease develops only in about 10 per cent of those infected. In most individuals, the body’s immune system will ‘wall off’ the TB bacteria, preventing it from multiplying and developing into active disease. This is known as latent TB, where the bacteria stay dormant for many years or even throughout a person’s lifetime.
In healthy adults with latent TB, 5 per cent go on to develop active TB disease within the first two years, and another 5 per cent may develop it sometime after two years or within their lifetime.
The progression from latent TB to active TB is more likely to occur if the immune system is weakened due to illnesses such as HIV infection, kidney failure, diabetes, and chemotherapy for cancer treatment.
It is important to know that persons with Latent TB do not have symptoms and cannot spread TB to others.
What Are Some Symptoms Of Active TB Infection?
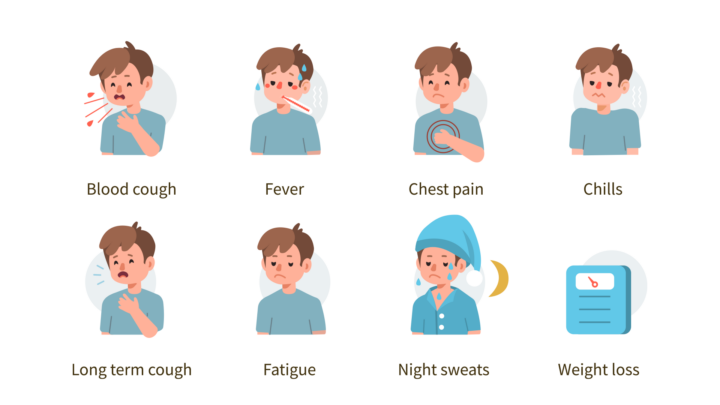
Symptoms of active TB disease include:
- Unexplained prolonged cough for three weeks or more
- Coughing up blood
- Low-grade fever or night sweats
- Fatigue
- Chest pain
- Weight loss
However, people with the active TB disease may have different symptoms depending on the infected parts of the body (e.g cough in pulmonary TB or back pain in spine TB)
Persons with active lung TB disease are infectious and can spread the disease to others unless treatment is started.
When Should One See a Doctor?
Persons with unexplained cough that persists longer than three weeks or exhibit any of the TB symptoms should see a doctor for evaluation. The doctor will then carry out further tests (blood tests, skin / sputum testing, chest X-Ray etc.) to determine if you have active TB disease.
Is the BCG Vaccination Good Enough to Prevent TB?
In Singapore, all children receive the Bacillus Calmette-Guerin (BCG) vaccine as part of the National Childhood Immunisation Programme. However, the vaccine only protects against very serious forms of TB, such as TB meningitis (TB of the brain lining). While the BCG vaccination provides some protection against lung TB, the protection is insufficient and lung TB can still occur. Booster doses have not been shown to provide added benefits.
How is Active TB Disease Treated?
Active TB can be treated very effectively with a combination of up to four drugs for six to nine months Once treatment starts, the person will rapidly become non-infectious and no longer pose as a source for infection. There is no further risk of exposure in the workplace or school, and there is therefore no need for workplaces or places where a recently diagnosed active TB case disease has visited to be closed.
What Happens if a Patient Does Not Adhere to Treatment?
Most people with active TB disease do not need to be hospitalised, but are required to go for Directly Observed Treatment (DOT) under the national TB programme. The DOT programme requires them to take TB medication under the direct observation of a nurse. It is important that persons with active TB disease adhere to and complete their treatment regimen even if they start to feel better after the initial period of treatment.
Stopping treatment or skipping doses can make TB resistant to medicines, leading to the higher chance of relapse and development of drug resistant TB. In such situations, a stronger and different set of drugs with more side effects must be taken for 18 to 24 months. There is also a lower chance of cure for drug resistant TB.
How Can TB Be Prevented?
- Persons who have been in prolonged contact with someone diagnosed with TB should visit the doctor for evaluation. To ensure early detection and treatment, and to curtail the spread of TB, the National TB Programme (STEP) carries out contact tracing and screening of close contacts to ensure that those at risk of infection are tested and receive appropriate treatment.
- Prompt and completion of treatment for the infected is the most effective way to prevent spreading of the disease in the community.
- During the first two weeks of TB treatment, patients should stay at home and adhere to strict hygiene measures such as wearing a mask and avoiding close contact with family members. This will prevent unnecessary spread of the disease to others living in the same premise.
- Infected persons must cover their mouths with tissue when they cough, and the tissue should be placed in a closed bag when it is being discarded.
- Persons with chronic illnesses or weaken immunity systems who are diagnosed with latent TB infection should receive preventive medication to prevent the infection from developing into active TB disease. Only one type of medication, compared to four (for treatment), is taken without the need for DOT (for latent TB).


