Vaccinations for Adults
Vaccines have greatly reduced or eliminated many infectious diseases that once routinely killed or harmed infants, children and adults. However, the viruses and bacteria that cause these diseases still exist, and you can still get these diseases if you are not vaccinated.
Reasons for Vaccinations
Decrease risk for serious diseases
Adults, especially the elderly and those with serious illnesses, are at greater risk of contracting infectious diseases like pneumonia, shingles, and influenza. They may suffer more severe consequences and even death.
Protect yourself and your loved ones from diseases
Although you may have been vaccinated as a child, the protection from some vaccines can wear off. You may also be at risk for other diseases due to your job, lifestyle, travel or health conditions.
You can’t afford to get sick
You have a busy life and too many responsibilities to risk getting sick. Vaccines can help you stay healthy so you don’t miss work. If you can avoid getting sick, you will have more time for your family, friends and hobbies.
Getting recommended vaccines can give you peace of mind. You will have the best possible protection available against a number of serious diseases.
Vaccines Are Very Safe
- Vaccines are tested and monitored. Vaccines go through years of testing before the Health Sciences Authority issues a license for their use.
- Vaccine side effects are usually mild and go away in a few days. The most common side effects include soreness, redness or swelling where the shot was given. Severe side effects are very rare.
- Vaccines are one of the safest ways to protect your health. Talk with your doctor about the vaccines you should safely receive based on your health or other conditions.
- Vaccines can lower your chance of getting certain diseases. Vaccines work with your body’s natural defences to help you safely develop immunity to diseases. This lowers your chance of getting certain diseases and suffer from their complications. For instance:
- Hepatitis B vaccine lowers your risk of liver cancer.
- HPV vaccine lowers your risk of cervical cancer.
- Flu vaccine lowers your risk of flu-related heart attacks or other flu-related complications from existing health conditions like diabetes and chronic lung disease.
- Dengue vaccine will reduce the severity of dengue infection, reduce hospital stay and severity of dengue symptoms.
- Vaccines lower your chance of spreading disease.
- Some people in your family or community may not be able to get certain vaccines due to their age or health condition. They rely on you to help prevent the spread of diseases.
- Infants, older adults and people with weakened immune systems (like those undergoing cancer treatment) are especially vulnerable to infectious diseases. For example, newborn babies are too young to be vaccinated against whooping cough. Unfortunately, whooping cough can be very dangerous or even deadly for them. Pregnant women should get the Tdap vaccine during every pregnancy to help protect their babies from whooping cough. Anyone who is around babies should be up to date with their whooping cough vaccine.
Types of Vaccines Recommended for Adults
Viral hepatitis A is usually a self-limiting viral hepatitis caused by the hepatovirus that is transmitted via the faecal-oral route as in eating contaminated food. In children, the course is commonly subclinical meaning asymptomatic, but severity increases with age. Furthermore, it has low potential for chronicity and long-term complications. Infection affords lifelong immunity to the virus.
Dosing and frequency
Two doses given six to 12 months apart.
Hepatitis B
Viral hepatitis B is the major cause of chronic viral hepatitis. It is transmitted through contaminated blood or serous fluids, sexual transmission, and vertical mother-to-child transmission. Acute hepatitis B can lead to chronic infection in around 5 per cent of patients. Chronic hepatitis B is the identified cause of up to 80 per cent of all hepatocellular carcinoma cases worldwide.
Dosing and frequency
One dose given one and 6 months apart.
Human papillomavirus (HPV) is a virus that is transmitted by direct contact (mostly sexual), which infects the skin, leading to the development of skin or genital warts, and cancerous or precancerous mucosal lesions. Of the more than 100 HPV subtypes, 40 subtypes infect the mucosal epithelium. Of these, 16 subtypes are considered high risk or oncogenic, acting as carcinogens that lead to cervical cancer and other anogenital cancers. These include subtypes 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 68, 69, 73 and 82. The most common ones are subtypes 16 and 18, which account for 50 per cent and 20 per cent of cervical cancer cases worldwide respectively. Initial HPV infection is considered a necessary step in the oncogenesis of cervical cancer.
This vaccine is recommended for all women from nine years through 45 years of age. The tetravalent can be used in boys that prevents anal warts and anogenital cancer.
Types of vaccines available:
- Bivalent: two serotypes 16 and 18
- Tetravalent: 6, 11, 16 and 18
- 9 valent: 6, 11, 16, 18, 31, 33, 45, 52 and 58
Dosing and frequency
Children initiated at nine through 14 years old are given two doses 6 to 12 months apart.
For ladies whose first dose is initiated at age 15 years or above, a three dose schedule is used at between two and six months.

Human influenza is a highly infectious respiratory viral illness with three types: influenza A, B and C. Influenza A and B are known to cause moderate to severe disease and epidemics, while influenza C causes a mild upper respiratory disease that does not lead to epidemics. The clinical picture of influenza includes fever, chills, headache, malaise, myalgia, anorexia, and respiratory symptoms (such as sore throat, cough and nasal discharge). Elderly patients may also present with confusion.
There are two types of vaccines available – the trivalent (three strains) and quadrivalent vaccine. The World Health Organisation recommends the use of the quadrivalent vaccine. The influenza virus undergoes substantial antigenic changes that leads to the emergence of different strains from year to year. This changes, and waning antibody levels, leads to a possible lack of efficacy of vaccines for one type of strain against other strains. Thus, the vaccine is updated annually according to the prevalent influenza strains at the time and thus yearly vaccination is recommended.
Dosing and frequency
Once annually. Safe for use in pregnancy and particularly for adults in the elderly age group.
Streptococcus pneumoniae can cause invasive pneumococcal disease (IPD), and capsular polysaccharides are the primary basis of its pathogenicity.
IPD can manifest as bacteraemia, meningitis, bacteraemic pneumonia or sinusitis. Invasive disease is most common in children four years old or younger but incidence slowly rises starting age 35 years. Patients aged 65 years and above are at high risk of morbidity and mortality.
The adult pneumococcal vaccines intended to prevent IPD and pneumonia that are available in Singapore are a 23-valent polysaccharide vaccine (PPSV23), and a 13-valent conjugate vaccine (PCV13) (Table 13).
Dosing and frequency
For patients age 65 years and above with no previous vaccinations either with PCV13 or PPSV23.
Start with PCV13 followed by PPSV23 six to 12 months later.
For those with illnesses or have been vaccinated before, please consult with your doctor regarding dosing regimen.
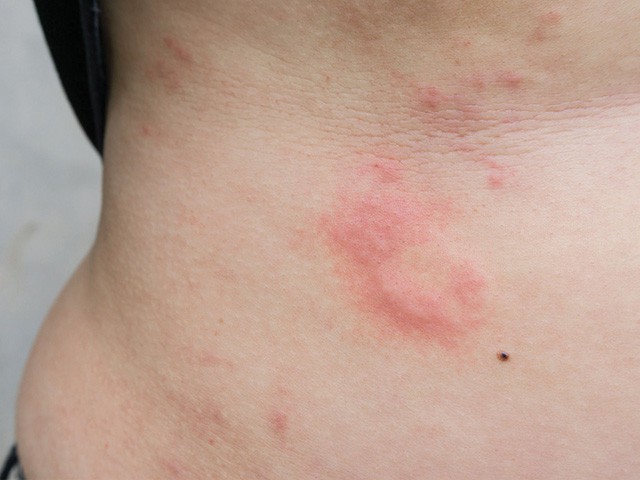
Shingles is a particularly debilitating illness for the elderly. It can cause eye diseases like corneal ulcers and vision loss.
It can also cause pneumonia and encephalitis. Most commonly, it causes severe pain in the elderly which is extremely debilitating.
Dosing and frequency
Shingrix: 90 per cent effective in preventing shingles. Comprise two doses two to six months apart
Zostavax: reduces risk of shingles in people above 60 years old by 50 per cent. One dose required only.

Dengue, as we all know is an endemic in Singapore and we are currently faced with a dengue epidemic.
This illness can cause high fever, severe headache and body aches, joint pains, skin rashes, nausea, vomiting, bleeding and even death.
Prior dengue infection will not protect you from future infections. The subsequent infection will increase your risk of dengue haemorrhagic fever or dengue shock.
There is now a vaccine available named Dengaxia. This vaccine has been proven to be clinically safe and has been shown to reduce severity of subsequent dengue by 95.5 per cent, reduce hospitalisation by 81.3 per cent, and reduction in symptoms by 81.9 per cent.
Dosing and frequency
For patients 12 to 45 years old with evidence of previous infection (documented, verifiable records of positive dengue antibodies or blood test for dengue antibodies).
Please consult your family physicians or travel clinics for more details on vaccinations.



